The Research Behind Physical Therapy for Sciatica
Sciatica is one of the most mismanaged conditions in outpatient medicine. People rest too long, stretch the wrong direction, or get sent straight to imaging without understanding what’s actually going on. The research on physical therapy for sciatica is both robust and underused — and it points in a clear direction.
Sciatica isn’t a diagnosis. It’s a symptom. That burning, shooting pain from your lower back through your buttock and down your leg? That’s a nerve being compressed or irritated somewhere along its path. The most common culprits are a herniated lumbar disc pressing against the nerve root, or piriformis syndrome — where a tight muscle in the buttock clamps down on the sciatic nerve directly. Treatment depends on which one is happening, and PT is built to figure that out.
A systematic review published in The Spine Journal found that physical therapy significantly reduced pain and disability in patients with lumbar radiculopathy — the clinical term for sciatica — with improvements that held up at 12-month follow-up. That’s not just short-term relief. That’s durable change.
A separate review in the Journal of Orthopaedic & Sports Physical Therapy found that directional preference exercises — movements tailored to how your specific nerve pain behaves — outperformed general stretching for reducing leg pain intensity. Not all PT is the same. What works for one person’s sciatica can make another person’s worse.
The research on surgery versus PT for sciatica is closer than you’d think. A landmark study from the New England Journal of Medicine found that outcomes for discectomy and conservative care — including physical therapy — were similar at two-year follow-up for many patients. Surgery got people out of pain faster in the short term. But PT caught up. And PT doesn’t carry surgical risk.
Early intervention matters. Research published in Spine journal shows that patients who started physical therapy within four weeks of sciatica onset had better long-term outcomes than those who waited three months or more. The nerve pathway doesn’t heal faster when you wait. It just gets more irritated.
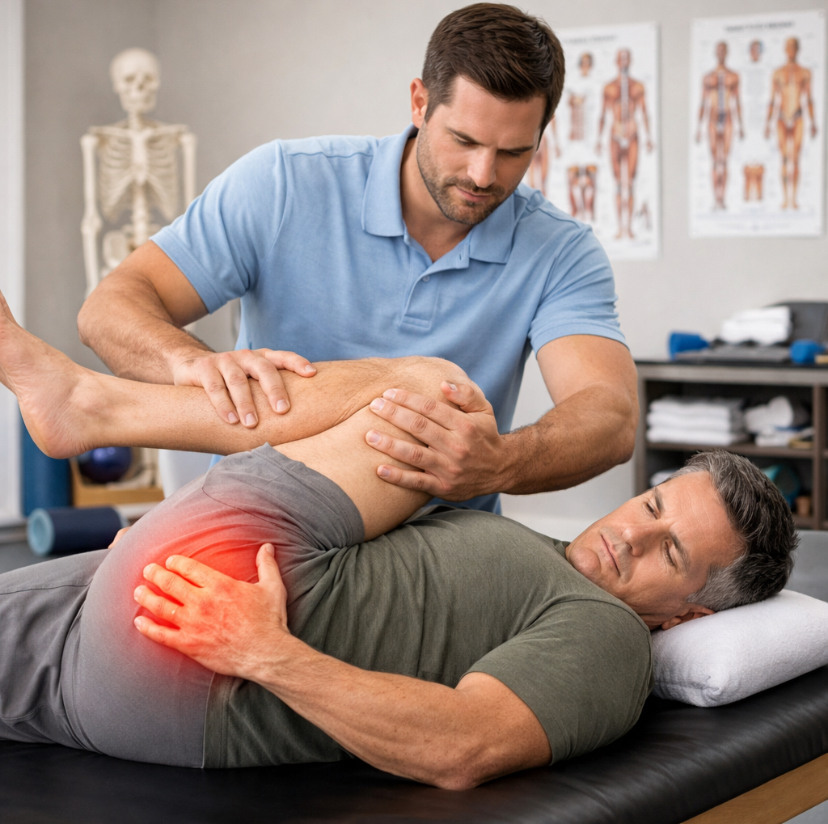
Physical Therapy Techniques Used for Sciatica Treatment
Not all physical therapy looks the same. What a therapist does for your sciatica depends on what’s actually causing it — a herniated disc is treated differently than piriformis syndrome, even though both can produce that same burning, shooting pain down your leg.
Manual Therapy
Manual therapy means your therapist uses their hands directly on your body — joint mobilization, soft tissue work, and sometimes spinal manipulation. The goal is to reduce pressure on the sciatic nerve by improving how the joints and surrounding muscles move. According to a review in the Journal of Orthopaedic & Sports Physical Therapy, manual therapy combined with exercise produced better short-term outcomes for lumbar radiculopathy than exercise alone.
Therapeutic Exercise
This is where the real, lasting change happens. Therapeutic exercise for sciatica focuses on strengthening the muscles that support your lumbar spine and pelvis — glutes, deep core stabilizers, hip flexors. When those muscles do their job, there’s less mechanical stress on the nerve.
McKenzie Method exercises are commonly used for disc-related sciatica. Research on physiotherapy management of sciatica supports nerve mobilization techniques as a meaningful component of structured rehabilitation programs. But the wrong exercise at the wrong time can flare symptoms badly — this is why self-treating with YouTube videos carries real risk.
Neuromuscular Reeducation
Sciatica doesn’t just hurt. It changes how you move. People with chronic sciatic pain often develop compensatory movement patterns that create secondary problems in the hips, knees, and lower back. Neuromuscular reeducation retrains the body to move correctly again.
Modalities as Support Tools
Ultrasound therapy, electrical stimulation (TENS), and heat or ice application are sometimes used alongside the techniques above. According to the American Physical Therapy Association, passive modalities should support — not replace — active rehabilitation strategies for lumbar conditions. A session that’s all modalities and no active work is a session that’s not moving you forward.
Ready to stop guessing and start getting better? Call (713) 992-5916 or learn more about sciatica physical therapy services in The Woodlands, TX.
Frequently Asked Questions
Can physical therapy actually fix sciatica, or does it just manage the pain?
Physical therapy can do more than manage pain — it can address the root cause of your sciatica. Research shows that targeted PT reduces pain and improves function, with results that hold up a year later. The key is identifying what’s actually driving your symptoms first.
What is a common mistake people make when treating sciatica at home?
The biggest mistake is treating all sciatica the same way. Many people do generic stretches or exercises they found online — but sciatica from a herniated disc needs a different approach than sciatica from piriformis tightness. Doing the wrong exercises can make things worse.
How do I know when to stop waiting and see a physical therapist for sciatica?
If your leg pain, numbness, or tingling has lasted more than two to four weeks, it’s time to stop waiting. Rest alone rarely fixes sciatica — it just delays care. If symptoms are spreading down your leg, getting worse with sitting, or waking you up at night, those are signs the nerve needs real attention.
Does the heat and humidity in The Woodlands, TX affect sciatica symptoms?
Yes, it can. Many people in The Woodlands spend long hours in air-conditioned offices or cars, which encourages prolonged sitting — one of the biggest aggravators of sciatic nerve pain. Reduced outdoor activity during hot months also leads to tighter hip flexors and weaker core muscles, putting more pressure on the lumbar spine.
Will sciatica go away on its own without treatment?
Some mild sciatica cases do improve on their own, but that’s not a reason to wait and hope. Research from Harvard Health Publishing shows that roughly 40% of people will experience sciatica at some point in their lives, and recurrence is common without addressing the underlying cause.
What should I expect during my first physical therapy visit for sciatica?
Your first visit focuses on finding the source of your pain, not just treating symptoms. A good physical therapist will ask detailed questions, watch how you move, and test your strength and flexibility. You’ll leave with a clear picture of what’s causing your sciatica and a plan built around your specific pattern — not a generic protocol.


