Vertigo Is More Than Just Feeling Dizzy
Most people use the word “dizzy” to describe vertigo. But they’re not the same thing. Dizziness is a vague feeling — lightheaded, unsteady, a little off. Vertigo is something else entirely. The room spins. Or you spin. Even when nothing is moving at all.
Where Vertigo Actually Comes From
The most common type is called Benign Paroxysmal Positional Vertigo, or BPPV. It happens when tiny calcium crystals in your inner ear — called otoliths — break loose and drift into the wrong canal. The National Institute on Deafness and Other Communication Disorders explains how these false signals cause the brain to perceive spinning that isn’t happening. BPPV accounts for roughly 20–30% of all vertigo cases seen in clinical settings.
But BPPV isn’t the only cause. Vestibular neuritis is an inflammation of the inner ear nerve, usually triggered by a virus. Labyrinthitis affects both hearing and balance. Meniere’s disease involves fluid pressure changes in the inner ear and often comes with ringing or hearing loss. Then there’s cervicogenic vertigo — dizziness that originates from the neck, not the ear at all. Each one behaves differently. Each one requires a different approach.
What Vertigo Actually Does to Your Daily Life
Rolling over in bed becomes a calculated risk. Looking up at a shelf, bending down to pick something up, turning your head quickly in traffic — all of it can trigger an episode. According to the Vestibular Disorders Association, roughly 35% of adults over age 40 have experienced some form of vestibular dysfunction. Falls become a real concern. In older adults, vertigo is one of the leading contributors to fall-related injuries.
The Mistake People Make Early On
A lot of people wait too long. They assume vertigo will pass on its own, or they take medication that masks the spinning without fixing the underlying problem. Some medications for dizziness actually slow down the brain’s ability to compensate and adapt — making recovery take longer, not shorter. It can help to review home remedies for vertigo to understand what self-care options exist and where their limits are.
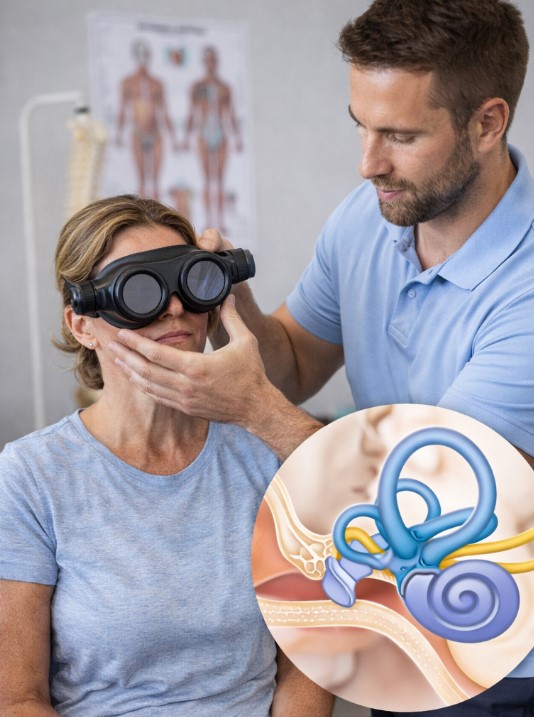
Physical Therapy Treats the Root Cause of Most Vertigo Cases
Most people who come to a clinic with vertigo have already tried something that didn’t work. A round of medication. A few days of rest. Maybe a trip to urgent care that ended with a referral and a shrug. What they haven’t tried is actually fixing the thing causing the spinning. That’s where physical therapy is different from almost every other approach.
The most common cause of vertigo is BPPV. According to the Vestibular Disorders Association, BPPV accounts for roughly 20% of all dizziness diagnoses seen in specialty clinics. In primary care settings, that number climbs even higher.
Research published in the journal Neurology found that the Epley maneuver resolves BPPV symptoms in roughly 80% of patients after one or two sessions. That’s not managing symptoms. That’s fixing the problem.
There’s also a category most people don’t hear about: cervicogenic dizziness. This is dizziness that originates from the neck. Tight muscles, joint stiffness, or nerve irritation in the cervical spine can all create a sensation that feels a lot like vertigo. A physical therapist who understands this connection can treat the neck directly — and the dizziness often resolves along with it.
According to the American Physical Therapy Association, vestibular rehabilitation therapy is a well-established, evidence-based approach for reducing dizziness and improving balance in people with inner ear disorders. That evidence base is why more physicians in the greater Houston area are now referring patients directly to vestibular-trained physical therapists instead of defaulting to medication first.
The Most Common Vestibular PT Techniques Explained Simply
Most people walk into their first vestibular PT appointment expecting to do balance exercises on a foam pad. What actually happens is usually more targeted — and more interesting — than that.
The Epley Maneuver
This is the one most people have heard of. If you have BPPV, the Epley maneuver is often the first thing your therapist tries. According to the American Academy of Neurology, canalith repositioning procedures like the Epley maneuver are effective for BPPV in roughly 80% of cases after one to three treatments.
The idea is simple. Tiny calcium crystals (called otoconia) have broken loose inside your inner ear and drifted into the wrong canal. That’s what triggers the spinning sensation when you roll over in bed or tilt your head back. The Epley maneuver moves your head through a specific sequence of positions to guide those crystals back where they belong. It takes about five minutes — and when it works, patients often feel a dramatic difference the same day.
Gaze Stabilization Exercises
This technique targets vestibulo-ocular reflex dysfunction — when your vestibular system has been damaged, your brain loses its ability to keep your vision steady when you move your head. Gaze stabilization exercises train your brain to compensate. You focus on a fixed target while moving your head back and forth. The neurological adaptation happening underneath is real — your brain is essentially rewiring how it processes movement signals.
Most guides skip over this: gaze stabilization only works if it’s dosed correctly. Too easy and there’s no adaptation. Too hard and you trigger symptom flare-ups that set the patient back. A trained vestibular PT adjusts the difficulty week by week based on how your symptoms respond.
Balance and Habituation Training
Some vertigo comes from a brain that has become overly sensitive to movement. Habituation works through repeated, controlled exposure to the movements that trigger your symptoms. Over time, your brain learns to ignore the false alarm. It’s uncomfortable at first. You may feel worse before you feel better. That’s expected — and it’s not a sign the treatment isn’t working.
Balance training focuses on retraining how your legs, eyes, and inner ear work together. Each exercise is designed to stress a specific part of your balance system so it adapts and gets stronger.
If you’re ready to stop guessing and start getting answers, call (713) 992-5916 or learn more about vestibular physical therapy in The Woodlands, TX.
Frequently Asked Questions
Can physical therapy actually fix vertigo, or does it just help you manage it?
Physical therapy can fix most vertigo — not just manage it. For BPPV, a repositioning technique called the Epley maneuver moves the loose crystals back where they belong. Many patients feel relief in one to three sessions. For other types, like vestibular neuritis, therapy retrains your brain to compensate. The goal is always to treat the root cause.
What should I expect at my first vertigo physical therapy appointment in The Woodlands?
Your first visit is mostly assessment. Your therapist will ask about your symptoms, when they started, and what triggers them. Then they’ll watch how your eyes move during specific head positions — that’s called a Dix-Hallpike test. It helps identify whether you have BPPV and which canal is affected. You may feel brief spinning during the test. That’s normal and expected.
Is it a mistake to wait and see if vertigo goes away on its own?
Waiting is one of the most common mistakes people make with vertigo. Some episodes do resolve on their own, but many don’t — and waiting gives the problem more time to affect your balance, your confidence, and your daily routine. Some medications used for dizziness actually slow your brain’s ability to adapt, making recovery take longer.
Does living in The Woodlands, TX affect vertigo or make it more common?
The Woodlands has a large population of desk workers and commuters on I-45. Long hours at a computer, poor posture, and the high rate of rear-end accidents in the area all contribute to cervicogenic vertigo, which comes from the neck rather than the ear. This type gets missed often because people assume vertigo is always an ear problem.
What is the difference between dizziness and vertigo?
Dizziness is a vague feeling — lightheaded, unsteady, or a little off. Vertigo is more specific. The room spins, or you feel like you’re spinning, even when nothing is moving. That difference matters a lot for treatment. Telling your therapist exactly what you feel — spinning versus floating versus unsteady — helps them identify the cause faster and choose the right technique.
How many physical therapy sessions does it take to treat vertigo?
It depends on the type of vertigo you have. BPPV often resolves in one to three sessions using repositioning techniques like the Epley maneuver. Other types, like vestibular neuritis or cervicogenic vertigo, may take several weeks of vestibular rehabilitation exercises. Most patients see meaningful improvement within the first two to four weeks.


